
Published on May 5, 2020 / Leer en español
Five things you should know today
1) Problems at the Postal Service
Analysis by Rosanna Torres, director of CNE’s office in Washington, D.C.
The United States Postal Service (USPS) is often mischaracterized as a quasi-governmental or private entity; it is neither. The USPS was established by Congress in 1971 (though its history dates back to its mandate in the U.S. Constitution) and operates as a self-run, government entity. Today, amidst competition from private competitors, the USPS is at the center of a large and expansive mailing industry. But its current state is very fragile.
Since 2007, USPS has experienced significant revenue losses that have affected its ability to manage its expenses. The situation has worsened with the coronavirus pandemic. Postmaster General Megan Brennan has warned Congress that the steady decrease in mail shipments combined with the economic fallout of the COVID-19 pandemic could drive the mail service out of business. The USPS expects a $13 billion revenue loss tied to the pandemic and an additional $54.3 billion over the next couple of years. Given the financial shortfall, the USPS is requesting $25 billion in direct emergency appropriations and another $25 billion to modernize the agency and make it more agile to respond to this new, highly uncertain environment.
2) Puerto Rico begins partial lifting of shelter-in-place restrictions
Puerto Rico began yesterday a partial lifting of the shelter-in-place restrictions that have been in effect since mid-March. The modified order allows the operation of certain retail establishments, the opening of professional service offices, and some construction and manufacturing operations, among other things. This even though the island’s Health Department has admitted its statistics about COVID-19 patients in Puerto Rico are flawed. Furthermore, the local press reports that several public health experts have doubts about the prudence of this decision, and some business owners say they don’t feel they have received adequate guidance regarding the safety protocols they have to implement during the reopening process.
The government also announced the creation of a working group that will be in charge of enforcing the new safety rules and protocols that apply to both individuals and business owners. If all goes according to plan, the second and third phases of the reopening of the local economy should take place in three-week intervals.
3) The Department of Health and Human Services and FEMA estimate U.S. COVID-19 death toll could increase to 3,000 per day
According to a document obtained by the New York Times, “deaths from the coronavirus over the next several weeks, [could reach] about 3,000 daily deaths on June 1”. As shown in the chart below, that would be a significant increase from the current rate of approximately 1,750 deaths per day.
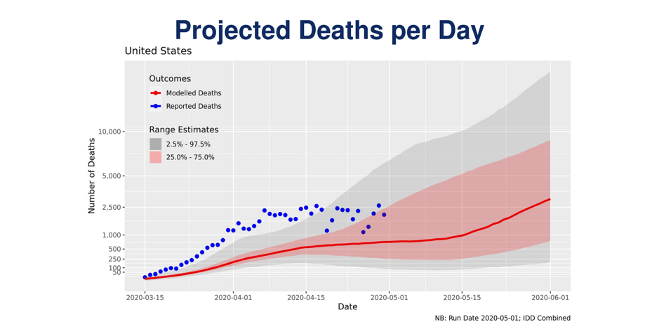
Unfortunately, “the projections confirm the primary fear of public health experts: that a reopening of the economy will put the nation back where it was in mid-March, when cases were rising so rapidly in some parts of the country that patients were dying on gurneys in hospital hallways as the health care system was overloaded.”
This is particularly worrisome as some states that have partially reopened “are still seeing an increase in cases, including Iowa, Minnesota, Tennessee, and Texas…[while] Indiana, Kansas, and Nebraska also are seeing an increase in cases and reopened some businesses on Monday.”
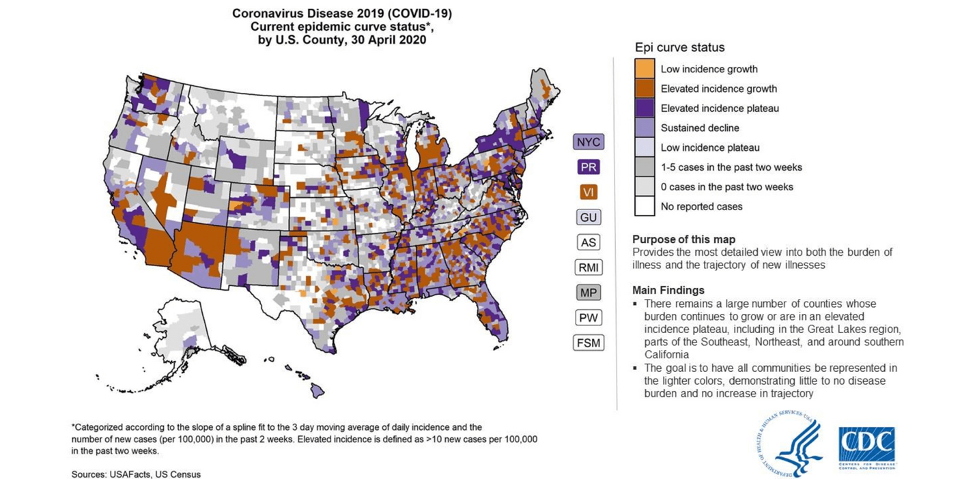
The White House has distanced itself from this model, even though it was created by its own administration, stating it has not been vetted. However, as Dr. Anthony Fauci pointed out yesterday, its value lies more in highlighting existing and future trends rather than on predicting exactly the number of new cases and fatalities, especially when many states are “leapfrogging” stages in the reopening. In other words, many states are proceeding with the reopening without meeting the minimum criteria for doing so. In that scenario, it is reasonable to expect a significant increase in both new cases and deaths.
Interestingly, in the case of Puerto Rico, as demonstrated in the chart above, the CDC believes the COVID-19 epidemic curve for the island to be in “an elevated incidence plateau status” which puts the island among those jurisdictions where the disease still represents a significant risk to the public health system.
4) R is the number
The reproduction rate or “R” number is “a measure of a disease’s ability to spread between people. It is the average number of new cases generated by an infected individual.” According to a recent article in the Financial Times, “if R is above 1, an outbreak expands exponentially — the higher the number the faster it grows. An R below 1 means the outbreak is contracting and, if it stays low, the disease will eventually die out.”
Epidemiologists estimate that for COVID-19, the “basic reproduction rate” in a population that has not been previously infected and has not implemented any restrictions is between 2.5 and 3. Until a vaccine is found, social distancing and shelter-in-place restrictions are the best policies for lowering R because keeping people apart reduces the probability that the virus will spread.
However, there are some caveats with the use of this indicator. First, most politicians use it as a proxy to measure the effectiveness of their policies, but R can vary from region to region in a country. So using an average R rate could be misleading because it could hide significant dispersion in infection rates across any specific jurisdiction.
Second, it is pretty hard to calculate. In theory, “an accurate value of R could be calculated by a very good testing and contact-tracing system, which would show the proportion of infected people who pass the virus on to someone else.” But in practice, very few countries have the capacity to do this well. Thus, scientists usually estimate R using mathematical models, but depending on the methodology, there could be significant variation in the results. Therefore, the results of those models should be interpreted with caution.
Nonetheless, even with its imperfections, this statistic is the best single indicator we have of how COVID-19 is spreading. Therefore, we can expect public health workers around the world to keep an eye on this number as countries proceed to lift shelter-in-place orders. This leads us to the question: do we know what the R number is for Puerto Rico?
5) What is contract tracing anyway?
Public health officials keep saying that contact tracing is a key element of any plan to lift shelter-in-place restrictions and relax social distancing orders. But what exactly is contact tracing? Fortunately, Vox has published a useful explainer.
According to the Vox report, contact tracing is “the difficult and sometimes tedious process of interviewing people diagnosed with COVID-19, finding out whom they have recently been in close physical contact with, and then informing those people of their potential exposure and advising them to self-isolate and get tested.”
This work is done by specially-trained workers, called disease intervention specialists, who have usually worked tracing outbreaks of sexually transmitted diseases, HIV, tuberculosis, and other infectious diseases. However, “tracing COVID-19 presents new challenges. One person infected with the virus can spread it to half a dozen others and symptoms often don’t present themselves for days after a person is already contagious.” Furthermore, “a respiratory virus like SARS-CoV-2 is also much harder to track than a sexually transmitted infection. The disease intervention team has to ask patients about everybody they’ve been in close proximity to since two days before they first felt symptoms from the coronavirus.”
In addition, contact tracing is a labor-intensive and expensive process: “The Johns Hopkins Center for Health Security estimated the US needs 100,000 people performing this work for state and local agencies. Former Centers for Disease Control and Prevention Director Tom Frieden told Politico the necessary number of workers could be as high as 300,000”; while some analysts estimate it would take “$3.6 billion to hire and train enough people to expand the disease intervention ranks, a figure endorsed by the Association of State and Territorial Health Officials.”
If we adjust the Johns Hopkins estimates for Puerto Rico, it will take 30 disease intervention specialists per 100,000 people, or 930 people to properly execute contact tracing in Puerto Rico. This leads us to the question: do we have the trained staff and the funding to perform this work in Puerto Rico?
Quote of the Day
“Every mistake is in a sense the product of all the mistakes that have gone before it, from which fact it derives a sort of cosmic forgiveness; and at the same time every mistake is in a sense the determinant of all the mistakes of the future, from which it derives a sort of cosmic unforgiveableness.”
—George F. Kennan
Note from the editor
In theory, three lines of defense should keep us safe, or at least prevent an unrestrained outbreak of COVID-19 in Puerto Rico as restrictions on daily life and commerce are lifted.
The first one is on us. Individuals have to keep practicing social distancing, wearing face masks, washing their hands, and avoiding large groups or gatherings. So far people have generally complied with these guidelines. It remains to be seen if they will keep doing so for the foreseeable future; it is one thing to wear a mask for a short period of time on a trip to the pharmacy or supermarket, it is quite another to wear it for eight hours at work.
The second line of defense depends on business owners and employers. They have to implement a safety protocol for each of their locations, provide their workers with protective equipment, modify working areas to provide adequate social distancing among and between workers, require their clients to comply with their safety guidelines and establish protocols for handling workers or clients that show up with symptoms—for example, a high fever. Business owners and employers have incentives to comply with these requirements, as people will avoid their stores or workplaces if they are not deemed safe. However, we do not know if they have adequate resources and guidance to fully implement these policies in workplaces across Puerto Rico.
The third and final line of defense is public health surveillance. Ideally, that would entail widespread testing and extensive contact tracing. In the absence of resources to execute those activities, Puerto Rico has to be strategic in the use of whatever resources it may have at its disposal. If the government waits until hospitals fill up, it will be too late, as the virus spreads exponentially. This means:
- testing healthcare workers and other first providers on a regular basis;
- having enough PCR test kits to test all persons with symptoms;
- proactively testing in locations with a high probability for an outbreak, such as nursing homes, prisons and manufacturing plants that cannot be modified to provide sufficient social distance; and
- randomly testing the population at large with antibody tests to get a better picture of how widespread the disease is in Puerto Rico.
Will it work? Well, we really don’t know. On the one hand, none of these defenses is perfect and each one has its defects. On the other hand, it is highly unlikely that all three will fail catastrophically. The hope is that each one will perform sufficiently well to make up for the deficiencies of the others, avoid a large outbreak, and keep new cases at a slow burn—that is, below hospital capacity.
But the virus is still out there and if we are not careful it will find us. To claim, by any objective measure, that Puerto Rico is prepared to withstand a large COVID-19 outbreak now or in the foreseeable future is, at best, wishful thinking. Puerto Ricans right now can only hope that the worst of this disease spares us.
This is the end of today’s briefing.
Stay safe and well informed!
